Vein Clinic:
‑ Ultrasound Evaluation‑ Sclerotherapy
‑ Mini‑Phlebectomy
‑ Endovenous Laser Therapy
Our Vein Clinic is a state-of-the-art facility providing the latest technological advances in vein treatment, specializing in Endovenous Laser Therapy.
More info...
Breast Cancer
Breast cancer is the most common cancer among women. In 1996, it caused 5,300 deaths in Canada.Every year more than 18,000 new cases of breast cancer are diagnosed. However, breast cancer is not limited to women. Women are about 100 times more likely to get breast cancer, but men can also develop breast cancer.
Known risk factors:
- age over 50 years old, hereditary (gene changes or mutations BRCA 1 and BRCA 2),family history of breath cancer, previous history of breast cancer, abnormal breast biopsy, menstrual periods - starting before 12 years old and menopause over age of 55), not having children, obesity.
There is variation in the diagnosis of breast cancer, depending if it is a palpable breast lump or an “abnormal” finding during screening mammogram.
If palpable, breast cancer can be diagnosed during physical (in the doctors office) or even self examination. In these cases, usually a suspicious lump is palpated. For further investigation a diagnostic mammogram or (and) an ultrasound are recommended. If a breast lump represent just a simple cyst (fluid collection), which completely disappears after aspiration – no other treatment usually is required. If a solid mass is diagnosed, breast biopsy will needs to be done and according to the results– treatment will be recommended.
Most “abnormal” findings identified during routine mammogram are not cancer. However more tests will be needed to make a diagnosis. First of all a physical examination is required to ensure that no breast lumps are palpated. Ultrasound can be valuable as well, particularly to distinguish between cyst and solid lesion. For further diagnosis stereotactic (under mammogram control) core biopsy or open biopsy using wire localization can be recommended. Again, treatment will depend on the results of the biopsy.
If no cancer is diagnosed - no further treatment is usually needed.
If cancer is found - the treatment options will vary according to the type of the cancer.
In case of Dustal Carcinoma In Situ (DCIS) or "non-invasive" cancer - the cancer is located within the milk ducts. It is less likely to spread and has a better outlook than "invasive" cancers. Usually wide local excision of the area involved is sufficient for the treatment. Sometimes radiotherapy will be recommended as well. In selected cases, for example with multilocal lesions - mastectomy can be recommended. Usually, there is no need to remove axillary lymph nodes for DCIS. Regardless the type of the treatment - wide local excision (breast conserving surgery) or mastectomy - survival rates are very high (between 95% and 100%) for 10 years after surgery.
In the case of Invasive Breast Cancer - the cancer is invaded the breast tissue outside the milk ducts.
In this case the treatment can be divided to local(for the breast) and systemic (for the whole body).
Local treatment includes breast conserving surgery (wide local excision with postoperative radiotherapy) and mastectomy(complete removal of the breast). The decision about the operation usually depends on the patient's preference (unless mastectomy is indicated). There is clear evidence that breast conserving surgery and mastectomy are equally safe and effective in removing the tumor and reducing the chances of the cancer returning.
 In the past, axillary lymph node dissection
was a necessary part of either operation as well.
Currently, it is recommended to perform an
Axillary Sentinel Lymph Node Biopsy
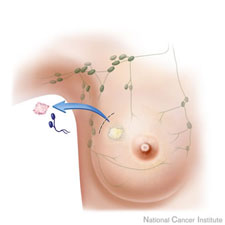
rather then formal lymph node dissection. During Axillary Sentinel Lymph Node Biopsy, we identify one or two lymph nodes (glands) that are first on the path of the lymph drainage from the breast. If no cancer cells are found at the sentinel lymph node – the cancer likely did not spread. Sentinel lymph node biopsy offers many advantages and allows us to avoid possible complications of lymph node dissection, such as injury to the nerves and axillary vein, numbness in the arm and postoperative lymphedema (swelling) of the arm.
In the past, axillary lymph node dissection
was a necessary part of either operation as well.
Currently, it is recommended to perform an
Axillary Sentinel Lymph Node Biopsy
rather then formal lymph node dissection. During Axillary Sentinel Lymph Node Biopsy, we identify one or two lymph nodes (glands) that are first on the path of the lymph drainage from the breast. If no cancer cells are found at the sentinel lymph node – the cancer likely did not spread. Sentinel lymph node biopsy offers many advantages and allows us to avoid possible complications of lymph node dissection, such as injury to the nerves and axillary vein, numbness in the arm and postoperative lymphedema (swelling) of the arm.Systemic therapy includes Hormonal Therapy (in case of estrogen and progesteron receptors positive cancers) and Chemotherapy (usually in case of high risk tumors or axillary lymph nodes involved by cancer).
A follow up with visits 6 months for 2 to 5 years after surgery is recommended. Regular self-examination is very important and should be practiced regularly. The first postoperative or "baseline" mammorgamm is performed usually about 6 months after surgery and then on the yearly basis.
Contact Us
Minimally Invasive Surgery:
‑ Appendix‑ Bowel
‑ Gallbladder
‑ Gastro‑esophageal Reflux
‑ Hernias
‑ Rectum & Anus
‑ Spleen
‑ Varicose Veins
Endoscopy:
‑ Gastroscopy‑ Colonoscopy
Other:
‑ Breast‑ Thyroid